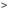Trending Now
- IPL 2024 begins with a bang. First contest between CSK and RCB.
- Election commission allots mike symbol to Naam Thamizhar Katchi
- AIADMK promises to urge for AIIMS in Coimbatore, in its election manifesto.
- Ponmudi becomes higher education minister.
Health Matters
Globally, there are approximately 9 million pregnant carriers of Thalassemia annually
![]() May 8, 2018
May 8, 2018
Thalassemia is the most common genetic based condition globally. The condition may be classified as a hemoglobinopathy which refers to genetic alteration causing structural abnormality in the hemoglobin molecule. Such defects lead to abnormal hemoglobin production and subsequent anemia. Symptom include tiredness, pale skin, bone problems, enlargement of spleen along with delayed growth and complications such as iron overload leading to cardiac, liver and immune system abnormalities.
Thalassemia is monogenic which means that a single causative factor is implicated in pathogenesis of the condition. Mediterranean, Middle East, Southeast Asian regions as well as the Indian subcontinent have reported high incidence of thalassemia as well as carriers of the condition. According to WHO statistics, globally, there are approximately 9 million pregnant carriers annually. About 56,000 new born children have a major thalassemia, including at least 30,000 who need regular transfusions to survive and close to 5500 affected die perinatally. Increasing rates of migration have also led to introduction of such genetic hemoglobinopathies into newer populations. Such new cases represent additional challenge to health services on a global scale.
Thalassemia exists in 2 major forms: namely alpha and beta thalassemia based on the hemoglobin chain that is affected. Other forms include delta and combination/compound heterozygosity variants. Beta thalassemia is further sub classified as beta-thalassemia major, intermediate and minor. Due to high frequency and severity, beta-thalassemia major is considered a major public health problem. This variant causes profound anemia that kills untreated affected children before the age of 3 years.
There is no effective treatment for thalassemia and the only way to prevent the condition is by detection of carriers and spreading awareness among the people about this emerging epidemic. Conventional treatments rely on regular blood transfusion and iron chelation therapy, or bone-marrow transplantation. Nonetheless, the financial burden and adverse effects associated with such therapies outweigh the benefits. Moreover, bone marrow transplantation calls for completely matched donors in order to minimize chance of rejection which is possible in only 25-30% cases. The need of the hour is newer therapeutic modalities that are safe and more effective which will enable affected individuals lead a normal life.
ALSO READ : World’s first 3D Sanskrit movie: In God’s own language, shot in God’s own country about God’s favourite dance form Koodiyattam
Regenerative medicine and cell based therapy have been studied in management of thalassemia with promising results. Mesenchymal stromal cells (MSC) are present in the bone marrow (along with hematopoietic-blood forming cells) and provide a supportive niche microenvironment to the affected hematopoietic cells. Additionally, MSCs are capable of self renewal and differentiation into various cell types thus have been implicated in maintenance of hematopoietic cells. Another interesting observation pertains to adipose tissue which has been described as an extra-medullary pool of functional hematopoietic stem and progenitor cells. Adipose derived cells may thus be researched as an additional possible source of hematopoietic cells.
A novel approach to hematopoietic stem cell transplant has been made possible by CliniMacs Prodigy System, which proposes un-matched/partially matched (haploidentical) transplants. Studies using this technology have shown that unrelated-donor stem cell transplantation is an acceptable therapeutic approach in severe thalassemia, especially for patients who are not fully compliant with conventional treatment and do not yet show irreversible severe complications of iron overload. This technology has already benefitted more than 5000 patients worldwide suffering from various hematological conditions.
“We have recently launched the first CliniMacs Prodigy System in India at our center with the hope of being able to effectively treat thalassemic individuals and also those suffering from other hematological disorders, malignancy etc. The aim is to reduce the waiting period for transplants and bring down the rate of mortality among affected individuals”, says Dr. Pradeep Mahajan of StemRx Bioscience Solutions Pvt. Ltd. “With a combination of mesenchymal cells for restoration of the bone marrow microenvironment and the CliniMacs Prodigy System, individuals suffering from thalassemia will be able to lead a normal life, free from major side effects associated with conventional modalities of treatment”, concludes Dr. Mahajan.